Root Canal Therapy (Endodontic Treatment)
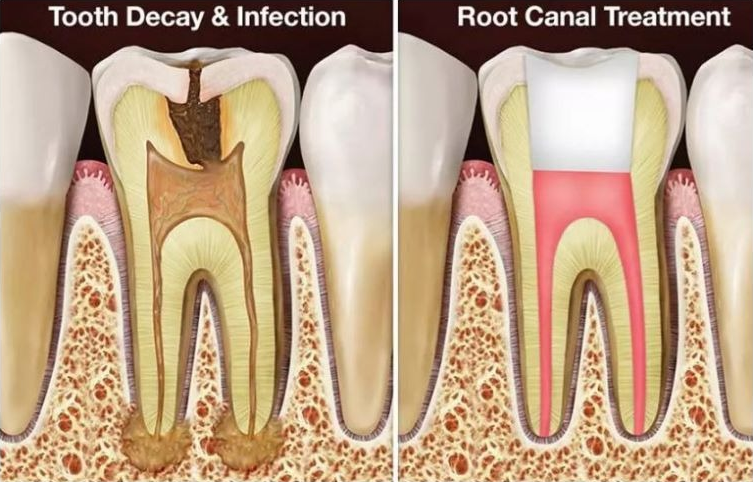
Root canal therapy (endodontic treatment) is a procedure used to treat infection or inflammation inside a tooth’s root(s) and to relieve pain while preserving the natural tooth where appropriate.
This page provides general information about the procedure, risks, expected outcomes, alternatives, costs, and practical details consistent with AHPRA and Australian dental regulatory guidance.
Who may need root canal therapy
- Symptoms suggesting inner tooth infection or irreversible pulp damage
- Persistent toothache or throbbing pain
- Sensitivity to hot or cold that lingers
- Pain on biting or chewing
- Swelling, gum tenderness, or a recurring pimple on the gum near the tooth
- X-ray evidence of infection or necrosis of the tooth pulp
- A clinical and radiographic assessment by a registered dentist or specialist endodontist is needed to determine suitability.
What the treatment involves
Initial assessment includes a clinical examination and dental radiographs (X-rays). Additional tests such as pulp vitality testing or bite tests may also be required.
- Local anaesthesia to numb the tooth and surrounding area.
- Isolation of the tooth with a rubber dam.
- Access opening to remove infected or inflamed pulp tissue from the pulp chamber and root canals.
- Cleaning, shaping, and disinfection of the canals using instruments and irrigants.
- Filling (obturation) of canals with a biocompatible material such as gutta-percha and sealer.
- Temporary or permanent restoration. A crown may be recommended to protect the tooth long term.
Treatment may require a single visit or multiple visits depending on the complexity of the case.
Possible benefits
- Relief of pain and removal of infection.
- Preservation of the natural tooth and its function.
- Avoidance of extraction where appropriate.
Risks and complications
- Not all treatments are successful; persistent or recurrent infection may occur.
- Possible complications include pain, swelling, fracture of instruments within canals, perforation, incomplete disinfection, tooth fracture, discolouration, retreatment, apicectomy or extraction.
- Medical or dental conditions, tooth anatomy, and patient factors affect outcomes.
- No guarantee of success can be given; realistic outcomes and alternatives will be discussed before treatment.
Alternatives
- Monitoring (if appropriate)
- Antibiotics alone for spreading infection or systemic involvement
- Extraction with replacement options such as implant, bridge, or denture
- Referral to an endodontist for complex cases
Before and after treatment
Please provide a complete medical history including medications, allergies, pregnancy, bleeding disorders, or cardiovascular conditions before treatment.
Some tenderness or discomfort may occur for a few days following treatment. Follow any oral hygiene, temporary restoration care, and dietary instructions provided by your dentist.
Follow-up appointments may be required to monitor healing and place a permanent restoration such as a crown if recommended.

